U.S. Military Suicide Prevention
The casualties of the wars in Iraq and Afghanistan are well known. But another cost has emerged: soldier stress, which can manifest itself in different ways.
One of the most troubling manifestations is suicide, which has increased among U.S. soldiers over the past decade. In response, the U.S. Department of Defense (DoD) asked researchers at the RAND National Institute for Defense Studies to review data on soldier suicide, identify what the scientific literature recommends and what leaders in the field consider to be the latest strategies for suicide prevention, and recommend ways to ensure that each service’s programs reflect the latest technologies. The results of the study are published in the book “The War Within: Suicide Prevention in the U.S. Military.”
Suicide in the military
RAND researchers examined the comparison of suicide rates in each unit with those in the civilian population, as well as the characteristics of those who have attempted suicide and those at risk of suicide.
What is the suicide rate in the military?
The defense forces only monitor the suicide rate of active duty military personnel. In 2008, the highest suicide rates were in the Army and Navy, with 18.5 and 19.5 suicides per 100,000 population, respectively; in the Air Force and Navy, 12.1 and 11.6 suicides per 100,000 population, respectively. In the Ministry of Defense, the number of suicides increased from just over 10 per 100,000 in 2001 to almost 16 per 100,000 in 2008, largely due to a statistically significant increase in the number of suicides in the military.
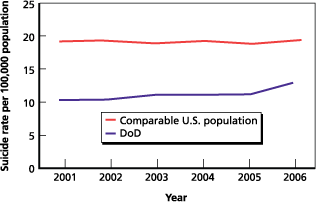
How does the military suicide rate compare to that of the U.S. population?
The annual suicide rate for the U.S. population is approximately 10 suicides per 100,000 people. Comparing the approximate U.S. figure to the military figure is misleading because the military population is very different from the general population. Therefore, the RAND research team calculated an estimated suicide rate for the U.S. population comparable to the military population in terms of age, gender, and race. The results of this comparison are presented in Figure [2]. The proportion of the comparable U.S. population is significantly higher than that of the military, but closing this gap remains a concern.
Who dies by suicide in the military and who is at risk?
There are a disproportionate number of men in the military, and men are generally more likely to die by suicide than women. According to the literature, the strongest predictor of death by suicide is a history of suicide attempts. Other predictors include mental disorders, substance abuse and substance use disorders, and head or brain injuries. However, none of these factors has strong predictive power, i.e., only a small proportion of people who attempt suicide or have a mental health problem die by suicide.
Research shows that “triggers,” i.e., events such as the death of a family member or the breakdown of a marriage or family relationship, only adversely affect people with an underlying vulnerability, such as a mental illness. There is some evidence to suggest that there may be a “contagion effect” (i.e., that a suicide or the reporting of a suicide may lead to other suicides), although it is thought to affect mostly those who are initially vulnerable. Evidence also consistently shows that the availability of firearms is associated with suicide.
Modern suicide prevention programs
The RAND investigators reviewed the evidence for a range of suicide prevention strategies, including those aimed at the general population, those that focus exclusively on at-risk groups, those aimed at making the environment safer, and those that are implemented after a suicide.
The authors’ assessment of these programs suggests that there are promising practices, but much remains unknown about what constitutes best practice, as there is little empirical evidence that programs or interventions have reduced suicide rates. However, any comprehensive program should achieve the following objectives:
Awareness and promotion of self-care. It may be important to focus on skill development at all stages of prevention and reduce known risk factors, such as substance abuse and mental health problems.
Identify high-risk individuals. A comprehensive suicide prevention program should include tools to identify high-risk groups, such as screening for mental health problems, one of the most important risk factors for suicide.
Facilitating access to quality care. Access to quality behavioral health care is an essential component of many suicide prevention programs. However, there are often a number of barriers to accessing such care, including the perception that behavioral care is ineffective or detrimental to an individual’s military career.
Providing quality care. The most effective empirical support for effective suicide prevention requires high-quality mental health services and suicide-specific interventions.
Restrict access to lethal means. Evidence consistently shows that restricting access to lethal means reduces the number of suicides. This applies not only to restricting access to firearms, but also to how potentially lethal medications are packaged and how door hinges and shower stalls are constructed.
Appropriate response. Because suicides can recur, suicide prevention programs should have a suicide response strategy that focuses on how the suicide is reported in the media and how the information is communicated to the groups to which the deceased belonged.
Suicide prevention in the armed forces and armed units
Apart from the armed forces, each service has different suicide prevention programs. The table lists the services’ activities according to six characteristics that must be reflected in the programs to be effective.
Recommendations
RAND researchers made 14 recommendations for strengthening suicide prevention programs in the military and across the services. Two of the 14 recommendations apply to all capabilities:
Conduct systematic and consistent tracking of suicides and suicide attempts. The recently implemented corps-wide suicide and suicide attempt tracking program will help ensure consistency of suicide information across the corps and promote information sharing among the services. However, the services and each agency should use the same criteria to determine which suicide attempts require follow-up reporting.
Evaluate existing programs and ensure that new programs include an evaluation component in their implementation. Evaluation provides a basis for decision making and ensures that resources are used effectively and that intended outcomes are achieved. Existing initiatives should be evaluated and an evaluation plan should be a mandatory part of all new initiatives.
The remaining recommendations are presented below according to the characteristics they seek to promote.
Raising awareness and promoting self-care.
Integrate skills training, particularly on help-seeking behavior, into awareness and self-care programs and initiatives. Most prevention programs focus on suicide awareness, information about resources for help, and sometimes messages to identify peers in need. More effort should be made to teach service members the skills they may need to reach out to mental health professionals or chaplains.
Identify suicide prevention issues and partner with agencies and organizations responsible for initiatives in other sectors. Each department’s suicide prevention programs should be linked to organizations responsible for other behavioral health issues identified as risk factors for suicide, such as mental health and substance abuse prevention, to ensure a consistent message, create jointly funded projects, and avoid duplication.
Identifying high-risk individuals.
Evaluate gatekeeper training. Services rely heavily on gatekeepers, individuals trained to identify people at risk for suicide and refer (or encourage them to go to) behavioral health providers or chaplains. There is no evidence that these prevention techniques are effective. Intuitively, it is attractive because it can reach a large number of people and help reduce stigma. On the other hand, it may send the message that suicide is always someone else’s problem, and some people are not good gatekeepers or are reluctant to refer their peers for fear that referral will have a negative impact on the referred soldier’s military career. Evaluation of these programs will help clarify these issues.
Develop prevention programs based on research and follow-up; the programs selected and recommended should be based on clearly identified, Army- and unit-specific risk factors. Most services produce reports describing the status of soldiers who have committed suicide, but do not identify the factors that actually put individuals at risk for suicide, which requires a well-defined control group. Identification of risk factors is essential for the development of prevention programs targeting at-risk groups.
Ensure that continuity of services and care is maintained when soldiers or their caregivers move from one institution to another, while respecting soldiers’ privacy and autonomy. Because Soldiers move frequently between installations and command posts and between active and reserve status, it is important that they are aware of the resources available at each new command post. Care should be taken to ensure that soldiers receiving care or counseling continue to receive it after they or their caregivers have been transferred. Mental health providers and chaplains can facilitate a successful transition by providing clients with the information they need to access resources at new installations and deployments, and by periodically reviewing their status as they relocate.
Facilitate access to quality care.
Inform soldiers of the benefits of using behavioral health care and the specific procedures and consequences associated with its use, and conduct research to provide information for dissemination. Many soldiers consider behavioral treatment ineffective and believe that seeking it may be detrimental to their careers. There is a lack of clear policy in the services about the consequences of seeking treatment, and research is needed to address these issues.
Where appropriate, military personnel need to be informed of the different behavioral health care providers available to them, including information about each provider’s qualifications, competencies, and confidentiality. Military personnel with behavioral health needs vary widely in terms of training, licensure, certification and credentials. Each unit also has chaplains who provide pastoral counseling. It is important to inform military personnel of the differences among deploying specialists. Since confidentiality is a particular barrier for this population and is not routinely offered by different service providers, military personnel should also be informed of the confidentiality offered by different professionals.
Improve coordination and communication between caregivers and service providers. Behavioral care providers should work as a team to ensure the emotional well-being of the individuals they serve. There are conflicting reports about the relationship between these professionals on military bases. Improving communication and collaboration between behavioral health providers and chaplains will help create a shift in trust so that individuals are not neglected as they transition from one form of care to another.
Determine if there are enough behavioral health professionals and chaplains with expertise in soldier mental health care. Messages promoted by behavioral health professionals and chaplains assume that there is adequate capacity to provide timely, quality care to those who request it. Anecdotal reports of a shortage of military chaplains and the known problems the Department of Defense has had in recruiting and retaining appropriately trained behavioral health providers underscore the need for research to address this issue.
Providing quality care.
Train primary care physicians, health care providers, and behavioral health professionals in evidence-based or up-to-date practices in behavioral health care in general, and suicide risk assessment in particular. Few behavioral health professionals have received adequate training on how to assess suicide risk and treat patients at different levels of risk. In addition, the provision of quality behavioral care is not common among these providers. The Navy and Air Force are taking some steps to train providers in suicide risk assessment and management, but efforts to improve the quality of behavioral care, such as training providers in evidence-based practices, are not integrated into the system of behavioral care delivered in military treatment facilities. There is little data on the quality of counseling provided by chaplains. Training all health care providers in mental health awareness and quality behavioral care is also an important part of health care provider training.
Limit the use of lethal means.
Develop creative strategies to limit the availability of lethal means among military personnel or individuals at risk of self-harm. Firearms play an important role in soldier suicides. Therefore, initiatives to limit access to firearms should be considered. The Veterans Health Administration and the Department of Defense have precedents for firearm restrictions. Strategies may include, in particular, adopting policies or procedures to restrict access to firearms, especially for those identified as at risk for self-harm.
Appropriate response
Provide commanders with formal guidance on how to respond to suicide and attempted suicide. An appropriate response to suicide not only helps to mourn the families of the suicide victim, but can also prevent potential copycat suicides and serve as a channel for dealing with high-risk individuals. No unit has direct guidelines on how a manager should respond to a suicide in his or her unit. In addition, some soldiers report being ostracized or ridiculed after seeking behavioral care or receiving treatment for suicidal behavior. This not only increases the risk of another suicide attempt, but also creates a hostile and stigmatizing environment for other unit members who may be under psychological or emotional stress. Leaders need guidance on how to deal with their units after a member has committed suicide, attempted suicide, or expressed suicidal thoughts.
Suicide is a tragic event, yet research shows that it can be prevented. These recommendations are ways in which, based on the best available evidence, some premature deaths could be avoided.
Comments
[1] Suicides among reservists who are not on active duty are not currently tracked.
[2] The most recent year for which data on suicides in the general population are available is 2006.
Read our general and most popular articles
- Diaetoxil
- Nuubu
- Regener 8
- CBD Vital
- Nordic Oil
- Potencialex
- Diaetostat
- Figur Kapseln
- Viscerex
- Prostaphytol
- Nutra Prosta
- Nutra Flex
- Diaetolin
- Matcha Slim
- Hepafar Forte
- Derila Kissen
- Exodermin
- HHC
- HHC Vape
- KU2 Cosmetics Hyaluronsäure Serum
- Liba Capsules
- KetoXplode
- Green Gummies
- Liver Ignite
- Ketoxboom Fruchtgummis
- Viagra Alternative
- Gundry MD Energy Renew
- ProDentim
- Phentermine Over The Counter
David W. Newton is a board certified pharmacist and also has been a board member for boards of examiners for the National Association of Boards of Pharmacy since 1983. His areas of expertise are primarily pharmaceuticals as well as cannabinoids. You can read an article about his expertise in CBD on the National Library of Medicine.
Reviewed by: Kim Chin and Marian Newton