Does VA have the necessary forecasting tools?
In 1996, the responsibilities of the Department of Veterans Affairs (VA) expanded significantly. The Veterans Health Care Reform Act of 1996 transformed the delivery of health care to veterans from an episodic provider of hospital care for veterans to a comprehensive health care provider covering all the medical needs of enrolled veterans.
To support budgeting and planning for this broader mission, a complex model called the Enrollee Health Care Projection Model (EHCPM) is used to project the future demand for veterans’ health care. Is the EHCPM up to the task? VA asked RAND (along with a senior independent actuary) to evaluate the model, which was developed and is used by an actuarial consulting firm. RAND’s evaluation focused on three key questions:
- Does the modeling support long-term budget planning and policy analysis?
- Does it accurately predict demand and costs for IL services?
- Is the model design and operation transparent to users and external parties?
The RAND evaluation found the EHCPM useful for short-term budgeting, but less useful for long-term planning, especially under alternative conditions. Fortunately, the model is structured in such a way that it can be modified to support long-term policy and planning applications without compromising its usefulness for short-term budgeting. The study also found that the high-level components of the model are relatively transparent, but the subcomponents of the model are much less so.
Key findings
RAND evaluated the model used by the VA to project future veterans’ health care demand. The evaluation found that
- The model is useful for short-term budget planning, but less so for long-term strategic planning and policy analysis.
- The model is structured in such a way that it can be modified to better support long-term planning and policy applications without compromising its usefulness for short-term budget planning.
- The high-level structure of the model is relatively open, but the elements of the model are less so.
How does the model work?
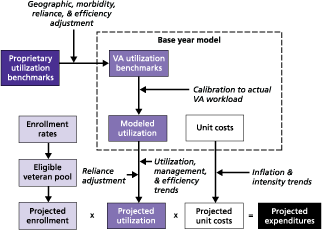
The EHCPM estimates veterans’ service utilization in the base year for each service category (e.g., hospitalizations, visits) using benchmarks based on commercial health plan utilization. The costs associated with the estimated utilization of each service are derived from data in the VA cost accounting system. In the next step, EHCPM estimates the baseline year of service utilization and the unit cost of services.
These estimates are based on expected changes in VA health care demand, the efficiency and intensity of health care provided by the VA system, and expected overall medical inflation in the United States. Each year, VA calculates expenditures for each service by multiplying expected enrollment, expected utilization, and expected unit costs (see figure).
Is the model a good example for budgeting and policy analysis?
RAND’s evaluation found that the EHCPM supports short-term budget planning and tracking in VA. The model identifies factors that affect a particular type of spending or type of insured spending and can be adjusted based on these factors if needed. The results of the model can help VA develop informed strategies for managing spending.
In addition, the current model allows VA to monitor budget execution and performance against pre-established benchmarks. The only thing limiting the usefulness of the EHCPM for these functions is the accuracy and timeliness of VA’s information systems, not the structure of the model.
However, for long-term strategic planning and policy analysis, the model can produce misleading results. The usefulness of the EHCPM in these types of applications is limited by two fundamental problems. First, in the current specification, the short-term usage projections are tied to the CA experience and thus do not measure the potential demand for services, which is independent of the current capacity of the CA delivery system.
Second, the current specification treats VA’s cost structure as a fee-for-service payer, such as Medicare or a commercial insurer, whose costs are highly variable. Therefore, if a significant portion of VA costs are fixed rather than variable, the predicted costs are unrealistic.
Using the model to develop scenarios beyond the current political and budgetary environment requires information on a wide range of factors, including the future cost structure of VA, how quickly VA can expand its capacity to meet demand, factors affecting enrollment, and relationships between enrollee health status, VA treatment options, and treatment preferences at VA facilities.
In many cases, needed data are missing or unavailable. Therefore, significant changes to model subcomponents and additional data are likely to be necessary before the EHCPM system can support long-term planning.
Is the model useful?
Does the model accurately predict the number of resources the VA will need in the coming years to meet projected demand? The accuracy of the model decreases when it is used to predict the impact of policy and budget scenarios beyond the current situation. The uncertainty is primarily due to the fact that the EHCPM cost projection is based on VA congressional appropriations and not an independent measure of resource needs.
Because of the discretionary nature of the VA budget, it is difficult to compare model projections to actual expenditures. In a discretionary budget, VA has no authority to spend more than Congress has appropriated. If the demand for VA services cannot be met with VA appropriations, the actual spending reflects the appropriations limitations and not the actual demand for VA services.
Is the model intelligible?
The overall structure of the model is relatively simple for users and external auditors to understand. However, the components of the model are less transparent. Transparency at this level is limited by several factors.
The complex algorithms used to determine the parameters of the model’s subcomponents; the inconsistent and often incomplete documentation of the model; the reliance on clinical effectiveness data and benchmarks that are proprietary to the EHCPM managing contractor and therefore not available for external review; and the lack of an ongoing process for external experts to obtain independent and periodic assessments of the model.
Recommendations for improving the model
To increase the utility of the model, the Veterinary Authority could consider modifying the subcomponents to more reliably forecast the demand and costs of veterinary care in a changing environment. This change would require significant investment to expand the research being conducted in CA and to develop new costing methods that include fixed costs. If these investments are not feasible, VA could consider simplifying the current model and making greater use of its own data resources.
A simpler model would be more transparent and could work just as well. For an improved or simplified model, VA could also consider other improvements, such as more accessible and complete documentation, involvement of more experts in model development, and periodic review by independent experts.
Read our general and most popular articles
- Diaetoxil
- Nuubu
- Regener 8
- CBD Vital
- Nordic Oil
- Potencialex
- Diaetostat
- Figur Kapseln
- Viscerex
- Prostaphytol
- Nutra Prosta
- Nutra Flex
- Diaetolin
- Matcha Slim
- Hepafar Forte
- Derila Kissen
- Exodermin
- HHC
- HHC Vape
- KU2 Cosmetics Hyaluronsäure Serum
- Liba Capsules
- KetoXplode
- Green Gummies
- Liver Ignite
- Ketoxboom Fruchtgummis
- Viagra Alternative
- Gundry MD Energy Renew
- ProDentim
- Phentermine Over The Counter
David W. Newton is a board certified pharmacist and also has been a board member for boards of examiners for the National Association of Boards of Pharmacy since 1983. His areas of expertise are primarily pharmaceuticals as well as cannabinoids. You can read an article about his expertise in CBD on the National Library of Medicine.
Reviewed by: Kim Chin and Marian Newton