Reservists are an integral part of the U.S. military and are constantly called upon to support operations around the world. Since September 2001, more than 800,000 reservists have been voluntarily and voluntarily called to active federal duty. Reservists in each unit are responsible for ensuring that reservists are not only properly equipped and trained, but also medically ready to enter service.
“Medically ready” means that service members have no health problems that would limit their ability to perform their duties, whether in the Reserve or on deployment. Medically ready reservists require fewer medical and dental services in the OR and fewer medical evacuations from the OR, saving money and freeing up resources for other purposes.
The Office of the Assistant Secretary of Defense for Reserve Affairs, concerned about potential gaps in medical readiness and inconsistencies in Individual Medical Readiness (IMR) requirements, asked RAND to suggest U.S. Department of Defense (DoD) policies that would help reservists achieve a higher level of IMR in the new operating environment.
The objectives of the study were to determine the current state of RC medical and dental readiness, identify barriers to achieving compliance, and identify alternative approaches to improving medical and dental readiness. The study also examined the costs associated with meeting current medical and dental readiness requirements and considered alternative approaches.
Key findings
- The Reserve Components have not met overall readiness goals, but have made progress in a number of areas.
- Barriers to achieving medical and dental readiness include the time and cost required to achieve readiness, the limited number of healthcare providers to assist members in meeting requirements, and inconsistencies in procedures.
- Opportunities for improvement include standardizing periodic medical examinations, modifying information reports, and including selected tests for conditions that may affect the reservist’s fitness for duty.
- Creative targeting of resources and offerings and the use of more group sessions could improve readiness levels and reduce costs.
Individual medical readiness
The concept of medical readiness is included in the specific requirements established by the MOD and the Armed Forces. Each member must undergo an annual physical exam, pass required medical tests, receive necessary vaccinations and be free of deployment-limiting conditions such as pregnancy, asthma and certain types of injuries. Each unit has its own approach to helping its RC members meet AMT requirements, receive immunizations and, if necessary, medical and dental care.
AMI is assessed through six measures: (1) PHA, (2) DLCs, (3) dental readiness, (4) immunizations, (5) medical laboratory testing, and (6) medical equipment. The military has established a minimum medical readiness goal of more than 75% of service members being fully medically prepared for these procedures.
RSC members have not met the overall readiness goal, but have made progress in a number of areas
The RAND study team’s analysis concluded that, although significant progress has been made in recent years, neither the active nor reserve forces have reached the Armed Forces’ goal of 75% of service personnel being medically fit. At the end of the second quarter of FY 2006, the Reserve Forces reported that only 26% of their personnel were medically fit, compared to 42% of the AC forces. By the end of 2009 (first quarter of FY 2010), 47% of Reserve Forces were fully medically ready, compared to 72% of CA Forces.
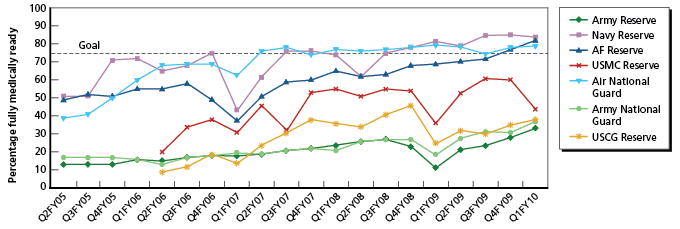
All RCs showed improvement. Figure 1 shows the percentage of members in full medical readiness in each RC from the second quarter of FY 2005 through the first quarter of FY 2010. The Air National Guard and Naval Reserve have met or exceeded the 75 percent target for full medical readiness since 2008; the Air National Guard met the target in the fourth quarter of FY 2009.
However, the two Army Reserve units have clearly struggled to meet the goal: they have never reported being more than 40% fully ready. The Coast Guard Reserve has performed only slightly better than the Army Reserve in recent quarters, and the latest figure for the Navy Reserve is also below 50%.
In some areas, significant progress has been made in meeting or approaching medical readiness requirements. For example, since the beginning of FY 2009, all at-risk communities have achieved over 84% compliance with DoD laboratory requirements, over 70% compliance with medical device requirements, and approximately 70% compliance with annual public health assessments. Vaccination compliance is also around 70% in all units except the Navy.
Barriers to AMI implementation are time and cost
The study identified several potential barriers to achieving and maintaining medical and dental readiness. These include the time and cost required to achieve medical readiness for reservists, the limited number of health care providers who can help members meet the requirements, and inconsistencies in procedures for achieving medical readiness.
Procedures for demonstrating compliance are not harmonized among installations or entities. Some units arrive at deployment locations in a different state because they have not received the required tests or treatment or because reservists’ health and dental records are not recorded in the medical management system.
Options for improving readiness
Most AMT requirements are generally adequate in the current operating environment. However, the study identified several opportunities to improve these requirements.
Standardize the PSA. The annual PSA assessment should be standardized so that all enrollees are assessed against the same medical criteria, just as they are assessed against the same dental readiness criteria. The Public Health Agency is currently working on standardizing the PSA.
Modification of data reporting and archiving processes. IMR data are not archived by the Defense Data Center or the services. Without standardized data collection and archiving, Defense cannot analyze trends or conduct retrospective studies.
Improve individual compliance. DOD should continue its policy of allowing reservists to receive TRICARE coverage for 180 days prior to deployment. Offering financial or other incentives, such as bonuses, for achieving readiness may improve IMR compliance.
Consider adding special testing for medical conditions that may impair reservists’ ability to perform their duties. For example, the military should consider screening for anemia in women, as significant iron deficiency can affect physical and mental performance. It should also ask questions about PSA that may reveal a pre-existing hernia.
Expand immunization and testing requirements. Services could include human papillomavirus (HPV) vaccination, cervical cancer screening and chlamydia testing.
Focus on demineralization (“repair and prevention”) rather than caries (“drilling, patching or removal”). Dental treatment that focuses on demineralization (the softening of tooth enamel that allows cavities to form) can prevent cavities. Dental fillings, remineralization therapy and chewing xylitol gum are effective in preventing and repairing tooth damage.
Cost of medical preparation
The study also analyzed the costs of different medical and dental preparation options. The researchers identified possible options in each area.
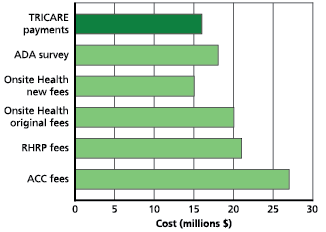
Figure 2: Estimated costs of dental care.
Options for improving dental preparation and reducing costs
To compare the cost of dental care under the different options, the researchers used data from the TRICARE Active Duty Dental Program (ADDP), which publishes monthly reports on payments made to TRICARE civilian providers for dental care preapproved and provided, as well as care received by Active Duty Dental Program members. The ADDP report for October through December 2009 shows that a total of 31 534 dental examinations and 180 175 dental procedures were paid.
For the 75 American Dental Association (ADA) codes competing for the latter contract, payments included administrative fees. Next, the researchers used prices from four other dental sources to calculate what the cost of each plan would have been for the total number of procedures documented in the ADDP report from October through December 2009.
The other four sources were the Reserve Military Health Readiness Program (RHRP), Onsite Health, which provides mobile health services to the National Guard in more than 40 states, ACC Consultants Inc, a small business that provides mobile dental services to soldiers, and the 2009 ADA Dental Charge Survey. The results are shown in Figure 2. The figure shows two Onsite Health fee-for-service rates: the initial rate (based on average prices) and the “new rates,” which represent the lowest possible price used to award a contract after a bidding process.
Figure 2 shows that all providers were more expensive than TRICARE, with the exception of Onsite Health’s “new rate.” This suggests that creative resource allocation and competition could improve current capacity levels and reduce costs. Since many new entrants need extensive dental care, dental readiness of new entrants could be improved through the use of contracted providers, such as Onsite Health or TRICARE dental rates. The two fee schedules provided by Onsite Health show the savings that can be achieved when working with providers to reduce costs.
Group dental visits are another cost-effective option. To calculate the cost of a group event, researchers created a “virtual unit” of 300 military personnel who participated in a two-day medical training weekend. Two contractors, RHRP and Onsite Health, reported their average costs for this dental readiness event: $271 and $332 per member, respectively. These costs include the personnel and equipment needed to perform dental examinations and some treatment procedures and to record data on the work performed.
The lack of standardization makes it difficult to estimate the cost of the PHA
As mentioned above, the application and requirements of the PHA (e.g., self-assessment questions and duration, list of “life activities” covered, requirements for members over 40 years of age) are not standardized across service units. This lack of standardization makes it difficult to estimate the cost of health information.
The researchers used prices from three vendors-Tricare, Onsite Health, and RHRP-to compare the cost of managing the individual PHI records of nearly 1,000 servicemembers. They used non-TRICARE (i.e., nonhospital) prices for physicians and nonphysicians (because PHI can be performed by a physician or other health care provider). The RHRP prices covered both inpatient and outpatient procedures.
A comparison of different IPS procedures shows that IPS can be improved and costs reduced. The table shows the costs of the five PHA procedures. The costs range from $98,640 for a PHA performed by a non-physician TRICARE outpatient provider to $169,232 for an RHRP clinical service. The most expensive provider is the RHRP clinical service.
The researchers also examined the costs associated with using small group work to perform HAP, as National Guard units typically do. The researchers calculated the cost of a hypothetical group session that included self-assessment, height, weight, blood pressure, pulse, vision, physical exam, cardiovascular exam, and electrocardiogram, as well as data entry for all services provided to 60 soldiers over the age of 40. RHRP and Onsite Health bid PHA exams for 300 members during that two-day event: the average cost per member was $121 for Onsite Health and $143 for RHRP.
Savings are likely to continue only if the DoD standardizes PHAs. The use of a standardized self-assessment form, combined with some annual health metrics, could help eliminate some of the disparities between the services and PHAs. Reserve organizations, in particular, would benefit from the development of a standardized “checklist” of needed medical services at an IMR team meeting.
This checklist would allow the unit to assess the need for reservist and contract support. This would greatly reduce the likelihood that essential services would be omitted from a subsequent contract.
Summary
This study has highlighted practices that have helped some reservists achieve full medical readiness and has identified cost-effective approaches to achieving and maintaining AMT. The military might also consider revising medical policies and procedures, including the requirement that reservists must meet AMI testing requirements to complete individualized advanced training or the basic officer training course. In addition, improved information sharing could help to better understand the requirements and better prepare for the AMT.
Read our general and most popular articles
- Diaetoxil
- Nuubu
- Regener 8
- CBD Vital
- Nordic Oil
- Potencialex
- Diaetostat
- Figur Kapseln
- Viscerex
- Prostaphytol
- Nutra Prosta
- Nutra Flex
- Diaetolin
- Matcha Slim
- Hepafar Forte
- Derila Kissen
- Exodermin
- HHC
- HHC Vape
- KU2 Cosmetics Hyaluronsäure Serum
- Liba Capsules
- KetoXplode
- Green Gummies
- Liver Ignite
- Ketoxboom Fruchtgummis
- Viagra Alternative
- Gundry MD Energy Renew
- ProDentim
- Phentermine Over The Counter
David W. Newton is a board certified pharmacist and also has been a board member for boards of examiners for the National Association of Boards of Pharmacy since 1983. His areas of expertise are primarily pharmaceuticals as well as cannabinoids. You can read an article about his expertise in CBD on the National Library of Medicine.
Reviewed by: Kim Chin and Marian Newton