Findings of New Cross-Over Surveys
As the United States withdraws troops from Iraq and Afghanistan and more soldiers return to civilian life, the military health care system must identify and manage the physical and psychological effects of war, which can persist long after deployment.
Among military personnel, comorbidities are common and are associated with an increased risk of post-traumatic stress disorder (PTSD), depression, suicide, cardiovascular disease, obesity, accidents and injuries, daytime sleepiness and fatigue. These problems can be detrimental not only to the health of the military, but also to the readiness of the troops.
However, most studies have focused on assessing one or a few aspects of sleep, usually sleep duration, and have ignored the many other dimensions of sleep. In addition, few studies have examined the independent effects of sleep problems on military health and readiness, in addition to other co-occurring risk factors, in a representative sample of military personnel from all branches and corps of the United States.
The RAND study – the first comprehensive study to assess the prevalence and impact of sleep problems in the U.S. military and to examine sleep-related policies and programs in the military – found that only 37 percent of soldiers get the recommended seven to eight hours of sleep per night and that nearly half of the sample had clinically significant sleep quality problems.
What are the factors that make sleep problems so prevalent in the military, and what are the consequences of sleep deprivation and other sleep problems in the military?
RAND researchers studied a large and diverse sample of married and deployed military personnel as part of the RAND Deployment Study, a longitudinal assessment of the antecedents, correlates, and consequences of family functioning during deployment. The results provide guidance for U.S. military and service policies and programs to identify, treat, and prevent sleep disorders and to maintain a healthy and ready force.
These problems can compromise not only the health of service members, but also the readiness of troops.
Sleep disorders are all too common among service members
Not only do service members rarely get the recommended seven to eight hours of sleep, but some 31 percent reported getting five hours or less, which is associated with a higher risk of mental and physical health problems. This rate is much higher than that of the general population: previous studies have shown that only about 8% of U.S. adults report sleeping an average of five hours or less.
However, civilian and military samples are often different. For example, civilian samples include more older people and women, but older people are expected to have more sleep problems, such as short sleep duration, rather than less.
The study also found that nearly half of the military sample scored above the threshold for clinically significant sleep problems on the Pittsburgh Sleep Quality Index (PSQI). In comparison, only one-third of the adult population had a PSQI score above this threshold.
The study examined in detail the sleep-related behaviors of military personnel
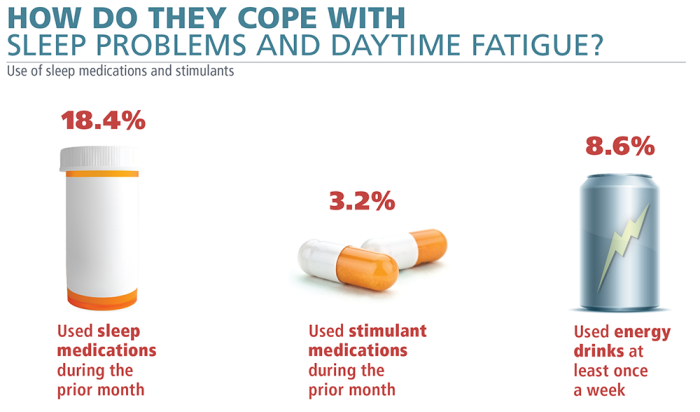
The RAND study assessed a variety of sleep disorders and examined sleep-related behaviors, such as stimulant and sleeping pill use. Especially in operational and training environments, it is not uncommon for soldiers to use stimulants such as energy drinks to stay awake during the day and sleeping pills to fall asleep at night.
A previous study conducted by the Joint Mental Health Advisory Group 7, which was created to assess the behavioral health and treatment of deployed troops, found that nearly 50% of deployed soldiers use energy drinks daily. However, it is less commonly known that service members use these products after they return home.
In the RAND sample, only 8% to 10% reported daily use of energy drinks, but the soldiers in the sample were generally older, all married, and most were not deployed at the time, which may help explain the differences between the RAND and Joint Mental Health Advisory Group studies. Use of sleeping pills was more common, with more than 18% of military personnel reporting use in the past month, which is consistent with the general population.
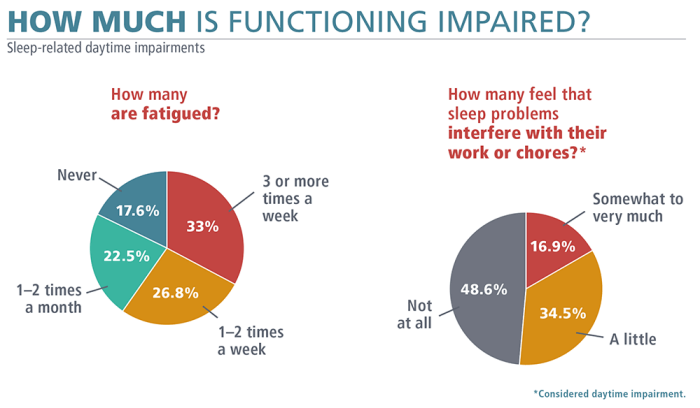
It is important to note that these medications have a wide range of side effects and their effectiveness and safety in the military setting have not been studied extensively. In addition, one-third of military personnel in the RAND study reported being tired at least three to four times per week, and approximately 17% reported that sleep problems interfered with their daily performance. These daily symptoms underscore the importance of sleep health in promoting military readiness.
Very little difference by deployment history
Sleep problems may be an inherent phenomenon of military culture, not just a consequence of deployment.
Surprisingly, there were few statistically significant differences in sleep problems or sleep-related behaviors based on whether the soldier had been deployed in the past, was currently deployed, or had never been deployed.
In contrast, sleep problems such as poor sleep quality, short sleep duration, and fatigue were common regardless of whether the patient had been referred elsewhere. This suggests that sleep problems may be an inherent feature of military culture and not just a consequence of deployment.
Sleep problems related to self-perceived health and ability
The study results showed that sleep problems-poor sleep quality, short sleep duration, fatigue, and daytime sleep deterioration-are associated with key health and performance indicators such as depression, PTSD, poorer physical health, and poorer unit readiness. These associations emerged even after statistically controlling for many other risk factors.
The findings regarding mental health problems are consistent with other studies of sleep in the military, but offer an even more conservative analysis when controlling for the many co-occurring risk factors. The study is also novel in that it assesses the impact of sleep problems on perceived readiness. These results also highlight the importance of considering multiple aspects of sleep rather than focusing solely on sleep duration. Indeed, poor sleep quality and daytime-related sleep deterioration were the most consistently correlated outcomes among the four outcomes.
Findings
In summary, the results of the sleep study indicate that members of the armed forces experience a wide range of sleep problems, including inadequate sleep duration, poor sleep quality, daytime fatigue and associated health problems, and compensatory behaviors such as the use of sleeping pills.
They also show that sleep disturbance is associated with negative mental and physical health outcomes and an increased risk of poor work performance, even when other factors associated with these outcomes are controlled for.
It is important to note that these analyses are based on data from a single survey wave and that the results are limited to married military personnel. Further longitudinal studies involving a sample of married and unmarried military personnel are needed to generalize the results to the entire military population and to examine the extent to which marital problems predict adverse health outcomes and decreased performance among military personnel.
Future research should determine whether evidence-based prevention and intervention strategies to promote sleep health can reduce the risk of later outcomes. If effective, these strategies could be an important future direction in promoting the health and readiness of the US military.
Filling key research gaps
- Members of the armed forces are more likely than the general population to suffer from a variety of sleep disorders.
- There are few statistically significant differences in sleep problems, suggesting that sleep problems are an inherent feature of military culture and not, for example, a direct consequence of deployment.
- Sleep problems are an independent risk factor for probable depression, probable PTSD, poorer physical health, and poorer unit readiness.
- These studies underscore the importance of identifying and treating poor sleep quality and duration in military personnel to reduce the risk of poor health and functioning and the impact on operational readiness.
Read our general and most popular articles
- Diaetoxil
- Nuubu
- Regener 8
- CBD Vital
- Nordic Oil
- Potencialex
- Diaetostat
- Figur Kapseln
- Viscerex
- Prostaphytol
- Nutra Prosta
- Nutra Flex
- Diaetolin
- Matcha Slim
- Hepafar Forte
- Derila Kissen
- Exodermin
- HHC
- HHC Vape
- KU2 Cosmetics Hyaluronsäure Serum
- Liba Capsules
- KetoXplode
- Green Gummies
- Liver Ignite
- Ketoxboom Fruchtgummis
- Viagra Alternative
- Gundry MD Energy Renew
- ProDentim
- Phentermine Over The Counter
David W. Newton is a board certified pharmacist and also has been a board member for boards of examiners for the National Association of Boards of Pharmacy since 1983. His areas of expertise are primarily pharmaceuticals as well as cannabinoids. You can read an article about his expertise in CBD on the National Library of Medicine.
Reviewed by: Kim Chin and Marian Newton