The mental health and cognitive health care needs of veterans
Since October 2001, some 1.64 million US troops have been deployed to Afghanistan and Iraq in support of operations. Many of them have been exposed to long-term combat-related stress or traumatic events. Ensuring the mental health of these soldiers and veterans is an important part of ensuring the future readiness of our military and replacing and honoring those who have served our nation.
Following recent reports and media attention, there is great public concern about the treatment of war injuries. Several task forces, independent review panels, and the President’s Commission have examined the treatment of war injuries and recommended improvements. Policy changes and funding changes are already underway.
However, the pace of policy change has been faster than the knowledge needed to find solutions. Data on the mental health and cognitive needs of U.S. soldiers returning from Afghanistan and Iraq, the costs of mental health and cognitive disorders, and the treatment systems available for care remain fundamentally lacking.
Key findings
- Approximately 18.5% of US soldiers returning from Afghanistan and Iraq currently have post-traumatic stress disorder or depression, and 19.5% report having sustained a traumatic brain injury during deployment.
- About half of those who need treatment for these conditions seek care, but only slightly more than half of those who receive treatment receive at least adequate care.
- Improving access to quality care (i.e. scientifically proven treatment) can be cost-effective and improve recovery rates.
Understanding invisible wounds: a challanging research
The RAND Corporation conducted a comprehensive study of the mental health and cognitive needs of returning soldiers and veterans to begin to close these knowledge gaps. The study focused on three major conditions: post-traumatic stress disorder (PTSD), major depression and traumatic brain injury (TBI). Unlike physical injuries, these conditions affect mood, thoughts and behaviour, and often remain invisible to other soldiers, family and society.
In addition, the symptoms of these conditions, particularly PTSD and depression, can have a delayed onset – they can appear months after exposure to stress. The effects of traumatic brain injury are still poorly understood, leaving a large gap in understanding the extent of the problem or how to address it.
The RAND study addressed questions in three areas:
- Prevalence: what are the rates of mental health and cognitive disorders that soldiers face when returning from deployments to Afghanistan and Iraq?
- Health Care System: What programs and services are in place to address the health care needs of returning soldiers with PTSD, major depression, or TBI? What are the gaps in programs and services? What steps can be taken to address these gaps?
- Costs: What are the social costs of these diseases? How much would it cost to provide quality care to all who need it?
Approximately one-third of returning soldiers report symptoms of mental health or cognitive conditions
The survey of recently returned soldiers was drawn from all those who participated in Operations Enduring Freedom and Iraqi Freedom, regardless of branch of service, component or unit type. Random sampling was used to reach a representative sample in the target areas. All participants were guaranteed confidentiality; the survey data will not be linked to any individual’s public records. A total of 1 965 people responded to the survey. The results showed that
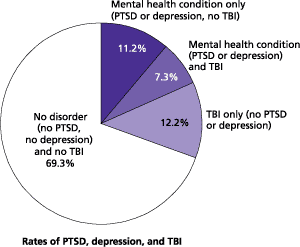
- 18.5% of all returning soldiers meet the criteria for either PTSD or depression (see Figure 1); 14% of returning soldiers currently meet the criteria for PTSD and 14% for depression (numbers not shown in Figure 1).
- 19.5 percent reported having a probable TBI during deployment (see Figure 1).
- Approximately 7 percent meet the criteria for mental illness and also report a probable TBI.
If these figures are representative, the study estimates that of the 1.64 million veterans deployed to date, approximately 300,000 veterans returning from Iraq and Afghanistan are currently suffering from post-traumatic stress disorder or major depression, and approximately 320,000 may have experienced a TBI during deployment.
Many services are available, but there are gaps in treatment systems
What programs and services exist to meet the needs of returning soldiers with these conditions? What are the gaps? How can the gaps be filled? To answer these questions, the RAND Task Force examined systems of care, identified gaps in care and barriers to care, and assessed how best to address these gaps.
Figure 1: An estimated 31% of soldiers returning from Iraq and Afghanistan have a mental health problem or have reported a concussion.
Availability gaps
The capacity of the Department of Defense and the Veterans Administration to provide health services has increased significantly in recent years, particularly in the areas of mental health and TBI. However, gaps remain in the availability and quality of services. There is a large gap between the need for mental health services and their utilisation.
This is due to structural factors, such as the availability of providers, as well as personal, organisational and cultural factors. For example, soldiers report barriers to seeking treatment related to fear of negative consequences of using mental health services. Survey results (Figure 2) suggest that most of these fears are related to confidentiality and career issues, making them particularly relevant for active duty service members. Many felt that seeking mental health treatment could undermine career prospects or undermine the trust of colleagues.
However, the VA also faces challenges in providing services to returning service members who may have to wait a long time for an appointment, especially at facilities whose resources are primarily geared toward the needs of older veterans. Better projections of the volume and type of demand from new veterans are needed to ensure that the VA has adequate resources to meet potential demand.
These gaps in access to care result in significant unmet care needs. According to our survey, only 53 percent of returning servicemembers who met criteria for PTSD or major depression sought help from a provider to treat these conditions in the past year. The gap is even larger for those who reported that they likely had a brain injury: 57 percent had not been seen by a doctor for a brain injury.
Quality gaps
The survey identified gaps in the provision of quality care. Only just over half of those with PTSD or depression who sought treatment received at least adequate care (defined by duration and type of care received). The number receiving quality care (care supported by scientific evidence) would be even lower.
The study also found gaps in the capacity of care systems to promote and monitor quality care. In particular, there is room for improvement in the organisational tools and incentives that support the provision of quality mental health care. Without these institutional supports, it is not possible to monitor that quality care is provided, including evidence-based care that is also patient-centred, timely and effective. DOD and the VA have begun training providers on evidence-based practices, but these efforts have not yet been incorporated into a broader system redesign that values and encourages quality care.
The VA has been a pioneer in promoting quality and can offer a promising model for improving the quality of mental health care in the DOD. Significant improvements have been observed in the quality of depression care provided by the VA, but an evaluation of the quality of care for PTSD at the VA is still ongoing.
Improving access to quality care can save money and improve services
If left untreated, PTSD, depression, and TBI can have far-reaching and damaging consequences. People with these conditions are at higher risk of developing other psychological problems and attempting suicide. They have more unhealthy behaviours – such as smoking, overeating and unsafe sex – and more physical health problems and mortality. People with these conditions also tend to miss more work or report being less productive.
These conditions can undermine relationships, break up marriages, exacerbate parenting difficulties and cause problems for children that can extend the consequences of combat trauma across generations. There is also a possible link between these conditions and homelessness. The damaging consequences of lack of treatment or neglect suggest that those affected and society as a whole would benefit greatly if more people received effective treatment.
These consequences can be of great economic importance, but most attempts to measure the costs of these diseases focus only on the medical costs to the state. However, the direct costs of treatment are only a fraction of the total costs associated with mental and cognitive illnesses. Much higher are the long-term individual and social costs of lost productivity, reduced quality of life, homelessness, domestic violence, family strain and suicide. Effective treatment and restoring veterans’ mental health to full capacity can significantly reduce these long-term costs.
It is therefore important to consider the direct costs of care in the context of the long-term social costs of inadequate care or lack of care. The RAND study sought to measure the total costs to society by taking into account the costs of care, productivity losses or gains and the costs associated with suicide. The study also calculated the cost impact of getting more people into care and improving the quality of care.
Estimates of the costs of PTSD and major depression over two years after deployment range from $5,900 to $25,760 per case. When these case-by-case estimates are applied to the proportion of the total population of 1.64 million soldiers currently suffering from PTSD or depression, we estimate that the total societal cost of these conditions is between $4.0 billion and $6.2 billion, depending on whether the cost of people who have lost their lives to suicide is included.
The cost per incident of TBI is significantly higher, but varies with the severity of the injury. The one-year cost estimate for mild TBI is $27,260-32,760 per case; for moderate and severe TBI, the cost estimate is $268,900-408,520 per case.
There is considerable uncertainty about the costs of TBI due to missing data; the total annual costs associated with diagnosed TBI cases (2,776 documented cases by mid-2007) range from $591 million to $910 million based on our calculations.
Although the costs of these conditions are high, we know that effective treatments are available, particularly for PTSD and depression. However, these evidence-based treatments are not yet available in all care settings. Our model also calculated the costs associated with PTSD and major depression if evidence-based treatments were more widely available (the effects of improving the quality of care for TBI are not well understood because there is a lack of long-term research on effective treatment and recovery rates).
- If 50% of people in need of treatment for PTSD and depression received treatment and all treatment was evidence-based, this greater investment in treatment would lead to overall cost savings (see Figure 3).
- If 100% of those in need of treatment for PTSD and depression received treatment and all treatment was evidence-based, the cost savings would be even greater. Costs for depression, PTSD or co-occurring PTSD and depression could be reduced by up to $1.7 billion, or $1,063 per returning veteran. These savings come from increased productivity and a reduction in the expected number of suicides.
Based on these estimates, evidence-based treatment for PTSD and major depression would pay for itself within two years. There are no reliable data on the costs of substance abuse, homelessness, family strain and other indirect consequences of mental health problems. If these costs were taken into account, the savings from effective treatment would be greater.
These results suggest that investing in evidence-based care makes sense for both society and the military as an employer. Sickness absence and recovery rates would increase, as would retention, productivity and readiness of soldiers and veterans.
Recommendations and conclusions
Taking all dimensions of our analysis into account, we make four key recommendations to improve the understanding and treatment of PTSD, depression, and TBI in military veterans:
- Increase and improve the capacity of the mental health system to provide evidence-based care. There are significant unmet needs in the treatment of PTSD and major depression among returning soldiers. DoD, VA, and civilian providers need additional treatment capacity, which will require new programs to recruit and train additional providers throughout the U.S. health care system.
- Changing policies to ensure that more soldiers and veterans seek the care they need. Many who need care are reluctant to seek it. Service members and veterans must have access to confidential services without fear of negative consequences.
- Provide evidence-based care in all settings. Providers in all settings should be trained and required to provide evidence-based care. This change requires the implementation of systems to ensure continuous quality and coordination of care and to support quality improvement in all settings where soldiers and veterans are served.
- Investing in research to address knowledge gaps and plan effectively. Medical science would benefit from a deeper understanding of how these diseases develop among veterans over time, and the impact of treatment and rehabilitation on outcomes. The United States needs a national strategy to support an aggressive research program that covers all medical services for this population.
Addressing the health care needs of returning veterans with PTSD, depression, and TBI is challenging. The prevalence of these conditions is high and may increase as the conflicts in Afghanistan and Iraq continue. Treatment systems have been improved to meet these needs, but critical gaps remain. Without effective treatment, these conditions will have significant long-term costs and negative consequences.
Ultimately, this problem extends beyond the DoD and VA to the overall US healthcare system and society as a whole. Many veterans seek care through private employer-sponsored health plans and in the public sector. The broader health care system must adapt to the needs of this population if the United States is to meet its obligations to veterans now and in the future.
Read our general and most popular articles
- Diaetoxil
- Nuubu
- Regener 8
- CBD Vital
- Nordic Oil
- Potencialex
- Diaetostat
- Figur Kapseln
- Viscerex
- Prostaphytol
- Nutra Prosta
- Nutra Flex
- Diaetolin
- Matcha Slim
- Hepafar Forte
- Derila Kissen
- Exodermin
- HHC
- HHC Vape
- KU2 Cosmetics Hyaluronsäure Serum
- Liba Capsules
- KetoXplode
- Green Gummies
- Liver Ignite
- Ketoxboom Fruchtgummis
- Viagra Alternative
- Gundry MD Energy Renew
- ProDentim
- Phentermine Over The Counter
David W. Newton is a board certified pharmacist and also has been a board member for boards of examiners for the National Association of Boards of Pharmacy since 1983. His areas of expertise are primarily pharmaceuticals as well as cannabinoids. You can read an article about his expertise in CBD on the National Library of Medicine.
Reviewed by: Kim Chin and Marian Newton